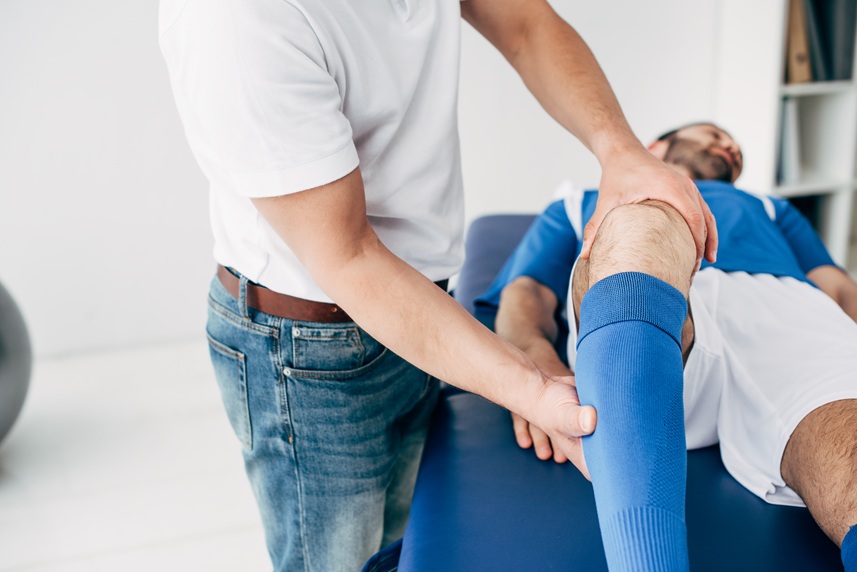
Do you want to return to running and sport safely? Let’s measure whether your knee is ready. At 12 weeks after meniscus repair, many patients reach a point where pain decreases, walking normalizes, and the natural question appears:
“Can I run? Can I resume training?”
The issue is that a repaired meniscus needs not only time, but also a knee that:
- moves fully
- does not swell after effort
- has sufficient strength (especially quadriceps and hamstrings)
- controls landing and loading on a single leg
That is why the 3-month assessment is a “safety filter” before increasing impact and intensity.
Who is this assessment for
- to return to normal walking (target from week 6 in your rehabilitation plan)
- to safely progress to more demanding exercises (advanced strength training, light jumping, running)
- to determine whether you can begin treadmill running (in your rehabilitation plan: starting from week 12)
Why the assessment matters (not just “12 weeks have passed”)
Modern rehabilitation protocols after meniscus repair are typically criteria-based and recommend progression according to clinical and functional signs (pain, effusion, mobility, control, strength), because the tear type and repair technique may sometimes require a more conservative approach.
The assessment is recommended if you are between weeks 4–12 after meniscus repair and want to:
This is also reflected in clinical practice: the gradual introduction of impact (running, jumping) depends on:
- a “quiet” knee (no swelling)
- full mobility
- sufficient strength
- good control during single-leg loading tasks
What we evaluate at the 12-week assessment (exactly as in your rehabilitation plan)
1) Mobility and tolerance (clinical criteria)
For returning to running, your rehabilitation plan requires:
- 95% knee flexion
- full extension
- absence of intra-articular effusion (no knee swelling)
Why this matters:
- Full extension is essential for efficient walking and proper load distribution
- Effusion after effort is a practical signal that the knee does not yet tolerate the stress dose; if it appears, progression must be adjusted
2) Muscle strength (minimum safety threshold)
Your rehabilitation plan uses a clear benchmark: at least 80% muscle strength compared with the healthy limb before running.
During the assessment, we compare left and right sides (as described in your rehabilitation plan):
- hip flexion
- quadriceps (isometric and isotonic)
- hamstrings (isometric and isotonic)
- gastrocnemius
- hip abduction and adduction
How we explain the percentage to patients (LSI)
LSI (Limb Symmetry Index) is calculated simply:
LSI = (performance of the operated leg ÷ performance of the healthy leg) × 100
Example:
- operated leg: 80
- healthy leg: 100
- LSI = 80%
LSI is widely used in knee rehabilitation as a symmetry benchmark between limbs.
3) Control and function: jumping and hop tests
Your rehabilitation plan includes functional criteria before running:
- pain-free running in water or AlterG (if used)
- pain-free jumping on the involved limb
- symmetric single-leg hop test
- similar triple hop test result
- countermovement jump
- squat assessment (equal loading)
- single-leg squat
Why these are important:
- Hop tests simultaneously measure power, neuromuscular control, and confidence on one leg
- The assessment evaluates not only jump distance, but also alignment, landing control, and equal loading
What follows after 3 months (progression from your rehabilitation plan)
.jpg)
Your rehabilitation plan clearly describes progression:
- from week 10: light bilateral jumping can begin
- from week 12: treadmill running can begin
In published rehabilitation protocols after meniscus repair, the exact timing may vary depending on the tear type and repair technique, but the logic remains the same: progression is gradual and individualized.
Why we perform this assessment at Centrokinetic
Between weeks 4–12, the objectives in your rehabilitation plan are very clear, and we translate them into measurable outcomes and concrete steps:
- increasing muscle strength (quadriceps, hamstrings, calves, glutes, adductors, hip flexors, lower trunk)
- movement quality (flexibility, proprioception, functional movement patterns: squat, lunge, step-up, running)
- physical conditioning and maintaining aerobic capacity with minimal joint stress
What you receive at the end
- clear criteria met or unmet for running (mobility, effusion, pain, strength, hop tests)
- objective strength and control percentages (symmetry)
- a structured plan for the next 2–4 weeks: what to increase, in what order, and what to monitor
- a recommendation for reassessment if needed
Frequently asked questions
If I am not in pain, can I start running?
Not automatically. Your rehabilitation plan requires clinical and functional criteria to be met (mobility, no effusion, at least 80% strength, hop tests).
Why is the absence of swelling so important?
Swelling is a signal that the knee has received more stress than it can tolerate; ignoring it increases the risk of setbacks in recovery.
Are hop tests safe?
Yes, when introduced gradually and at the appropriate time. They are well-established functional tools in knee rehabilitation.
Schedule your 3-month post-meniscus repair assessment
If you are approximately 12 weeks after meniscus repair and want to resume running without uncertainty, this assessment clearly shows whether you are ready and what still needs improvement.
Centrokinetic e locul in care vei gasi raspunsuri si solutii clare pentru problemele tale de motricitate. Clinica dedicata afectiunilor osteoarticulare e impartita in urmatoarele departamente specializate:
- Ortopedie, departament compus dintr-o echipa de medici ortopezi extrem de experimentata, condusa de Dr. Andrei Ioan Bogdan, medic primar in ortopedie-traumatologie, cu activitate chirurgicala la Spitalul de Ortopedie Medlife, specializat in traumatologia sportiva si in chirurgia gleznei si a piciorului.
- Ortopedie pediatrica, unde sunt tratate afectiunile sportive ale copiilor (leziuni ligamentare si de menisc), deformarile coloanei (scolioza, cifoza, hiperlordoza) si cele ale picioarelor (hallux valgus, hallux rigidus, picior var equin, picior plat valg, picior cav).
- Neurologie, ce dispune de un departament ultraperformant, unde sunt efectuate consultatii, electroencefalograme (EEG)si electromiografii (EMG).
- Recuperare medicala pentru adulti si copii, departament specializat in recuperarea sportivilor de performanta, in afectiunile coloanei vertebrale, in recuperarea copiilor cu afectiuni neurologice si traumatice. Experienta noastra este extrem de bogata, tratand peste 5000 de sportivi de performanta.
- Imagistica medicala, clinica fiind dotata cu ecograf si RMN, aparate performante dedicate afectiunilor musculoscheletale, si completata de o echipa experimentata de radiologi: Dr. Sorin Ghiea si Dr. Cosmin Pantu, specializati in imagistica musculo-scheletala.
- Reumatologie, departament complet care se ocupa cu diagnosticarea, tratarea si recuperarea bolnavilor cu afectiuni nechirurgicale ale aparatului locomotor.
- Chirurgie vasculara, departament coordonat de doamna dr. Neagu Cristina, medic primar chirurgie vasculara, supraspecializata in diagnosticarea si tratamentul bolilor sangvine, adica a arterelor, venelor si a vaselor limfatice.
Afla noutatile urmarind conturile de Facebook, Instagram si YouTube ale clinicii Centrokinetic.



















































































































































